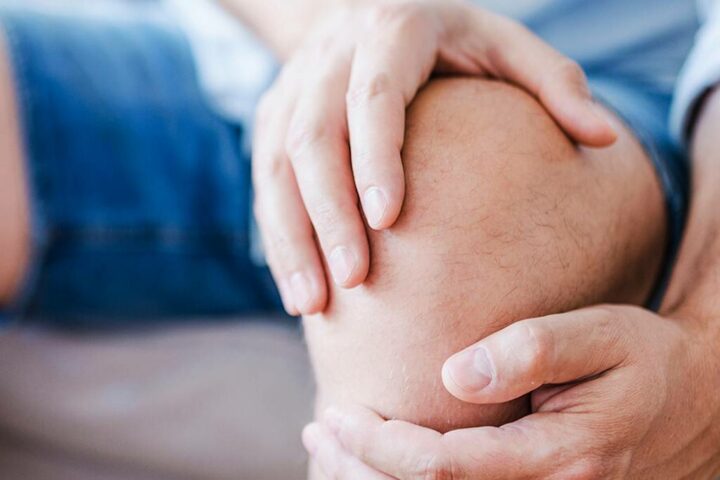
Algodystrophy, now better known as Complex Regional Pain Syndrome (CRPS) type I and II, is a multi-symptomatic loco-regional syndrome. It causes intense and continuous pain, located at the level of the lower or upper limbs and is generally associated with oedema. CRPS is not a tumour, but a highly painful disease, with a high probability of being treated if diagnosed in its early stages. The earlier the treatment, the lower the risk of disability.
In 50-70% of cases, algodystrophy is caused by trauma or surgery resulting in immobilisation; it is rarely related to ischemic brain or heart diseases, neoplasms or some infectious diseases. Sometimes spontaneous cases of algodystrophy can be observed that are not attributable to a triggering event at the affected site.
According to experts, there are two types of algodystrophy:
- algodystrophy type 1, also known as “complex regional pain syndrome I”
- algodystrophy type 2, or “complex regional pain syndrome II”
In cases where the disease has been preceded by nerve damage, it is referred to as algodystrophy II, type I if such damage does not appear recognisable.
Sometimes, complex regional pain syndrome type 1 (CRPS I) is referred to as reflex sympathetic dystrophy (RSD), shoulder-hand syndrome, Sudeck syndrome, or Algodystrophy. Instead, complex regional pain syndrome type 2 (CRPS II) is known as causalgia or algoneurodystrophy.
Where does algodystrophy hit?
Before focusing on its causes and its symptoms, let’s take a look at the parts of the body most commonly affected by this syndrome.
As already mentioned, algodystrophic syndrome mainly affects the lower and upper limbs.
- As for the former, among the most common forms are the algodystrophy of the knee and hip, but also that of the foot and ankle.
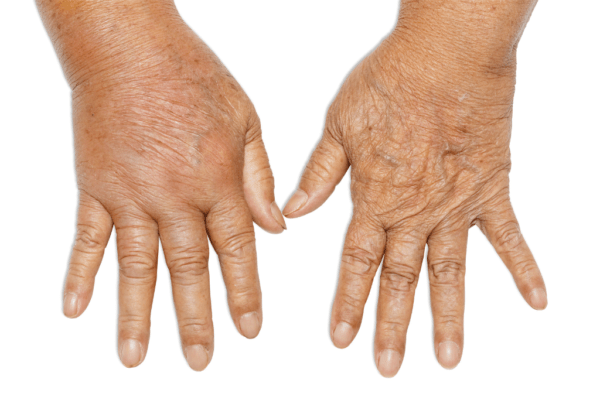
- When it is located in the upper limbs, algodystrophy mainly affects the hand and wrist.
Algodystrophy: causes
Algodystrophy seems to result from a disorder of the functioning of the sympathetic nerves.
As mentioned, it can arise as a result of trauma (fracture or distortion), surgery or without an apparent cause.
Despite this, the causes remain largely unknown.
However, some risk factors increase the chances of contracting the disease:
- neurogenic inflammation;
- dysfunction of the sympathetic nervous system;
- damage and/or dysfunction of the microcirculation, which causes local hypoxia;
- acidosis resulting from hypoxia related to localised osteoporosis;
- aberrant healing process.
Symptoms and diagnosis
It is difficult to diagnose algodystrophy because the symptoms are not very specific and may resemble those of other diseases and conditions.
Despite this, the presence of pain in a specific and circumscribed region is a signal that can guide the doctor towards the diagnosis of algodystrophy.
The characteristic symptoms are oedema, hyperalgesia, and in particular allodynia, abnormal sweating, hypertrichosis and reduced joint excursion with district osteoporosis; motor alterations may be associated which in some cases include tremors or abnormal postures.
After which, any further symptoms and the presence of previous trauma are evaluated, which can help to reach the diagnosis. We are talking about post-traumatic algodystrophy precisely because, as mentioned above, in most cases it is linked to trauma: distortion, joint fracture, crushing trauma or repeated microtrauma.
Other symptoms are related to skin discolouration, the skin appears warm and red and slowly may become cyanotic, and trophic alterations. Specifically, signs of altered trophism of the hair, scalp and nail growth and shine.
The symptoms of algodystrophy can be detected by an x-ray or, if they are more restricted to a single area, by an MRI scan or triphasic scintigraphy.
Scintigraphy is certainly the most appropriate examination because it can detect even minor bone changes compared to a radiographic examination.
Nevertheless, one drawback is due to the fact that the scintigraphic picture varies according to the different stages of the disease.
In addition to those already mentioned, blood tests and nerve conduction studies may be carried out, to exclude, respectively, the presence of rheumatological infections or diseases and damage to the nerves.
Therefore, no specific diagnostic test is foreseen and despite the possibility of using these tools, the diagnosis of algodystrophy is predominantly clinical.
Recommended therapies for algodystrophy
There is no specific treatment for algodystrophy and therapy includes treatments that have the sole purpose of alleviating the symptoms of the disease (symptomatic therapy).
As a result, it is not possible to talk about healing times for those suffering from algodystrophy. In many cases, the symptoms stop spontaneously within 6-18 months. But about 15% of patients may have pain that is resistant to therapy and reduced functionality up to two years after symptoms begin.
The three main types of therapy are looked at below.
Exercises to relieve algodystrophy
Rehabilitative treatment should be appropriate for the patient and started as soon as possible as soon as the diagnosis is made, to reduce pain, avoid contractures and capsular retractions and monitor the psychological status of the patient due to the painful symptomatology.
The treatment involves firstly the rest of the affected region and mobilisation. In particular, active and passive exercises allow to maintain joint mobility and flexion avoiding stiffness and loss of muscle trophism.

Physical therapy involves performing physical therapy exercises for the treatment and rehabilitation of the hand, hip, knee, foot and limbs in general. As a result, algodystrophy can lead to atrophy in the affected area. This is a late event in case of diagnostic/therapeutic delay, or in more severe cases where the response to treatments was partial or ineffective.
An example is mirror therapy (mirror therapy or mirror visual feedback), a technique in which the patient is asked to move the healthy limb, which is reflected on a mirror to give the impression that the affected limb moves without pain, gradually restoring movements. Or, vascular gymnastics with hot water and cold water to treat algodystrophy in the hands with rehabilitation exercises. Alternating hot/cold baths and ice are indicated for the reduction of oedema and swelling. However, they are to be advised with caution, due to alterations in peripheral sensitivity and vasomotor characteristics of algodystrophy.
Drug Therapy for Algodystrophy
Concerning drug therapy, doctors can prescribe a whole host of drugs:
- Non-steroidal anti-inflammatory drugs (NSAIDs): they are used to relieve pain by tackling inflammation;
- Corticosteroids: these are steroid anti-inflammatory drugs used in the early stages of the disease when the infection is evident. The administration is indicated for short periods, under medical advice, and is avoided for long periods for possible side effects.
- Anticonvulsants, are indicated to treat spasticity and neuropathy.
- Tricyclic antidepressants, are indicated to treat neuropathic pain.
- Opioids (e.g.: morphine): they are very powerful analgesics. Also in this case, as with corticosteroids, you should not exaggerate because they can lead to side effects.
- Local anaesthetics: they are used in the form of creams.
Psychological Therapy for Algodystrophy
Finally, psychological therapy, also called psychotherapy, is recommended by doctors to all people who have developed depression, anxiety or other psychological disorders resulting from the onset of algodystrophy.

Additional therapies to treat algodystrophy
There are other types of algodystrophy treatment, one of which is sympathetic nerve block. This therapy involves the injection of an anaesthetic near the spinal cord, to stop the activity of one or more nerves of the sympathetic nervous system. It is not effective in the long run, but it may be useful to temporarily reduce pain.
Algodystrophy and magnetotherapy
As far as instrumental physical therapy is concerned, magnetotherapy acts both on the painful symptom, calming it, and on the level of inflammation, reducing its effects. Thanks to the biostimulation of the cells, the process of communication between the inside and outside of the cell is reactivated, accelerating the healing times.
There are multiple magnetotherapy devices to treat algodystrophy. Once the one with the most suitable applicators for the area to be treated has been chosen, it is possible to carry out therapy with total autonomy.
Thanks to the therapeutic strap and the pair of solenoids it is possible to comfortably treat algodystrophy in the knee, hip or hands. If the affected area is the foot, it may be more comfortable to use the TAP2000 mat. If you have any doubts about which applicator is best to use for the area to be treated, you can download our I-Tech Life app at any time and consult the guide on solenoid positioning.
If you have been diagnosed with algodystrophy and your doctor has prescribed magnetotherapy treatments, you may be wondering which device is best for you. Then you’ve come to the right place! We offer a wide range of certified medical devices, suitable for every need.